COVID-19 pushes the trend toward office-based labs
- ByPolk & Associates
- Feb, 18, 2022
- Health Care
- Comments Off on COVID-19 pushes the trend toward office-based labs
COVID-19 has spurred innovation and growth, including the trend toward outpatient care at office-based labs. As a result of increased calls to keep patients out of the hospital and safe from infection during the pandemic, the Centers for Medicare and Medicaid Services has encouraged procedures in the outpatient setting, according to Lindsay Pack, Office-Based Labs […]
Confronting the Great Resignation: How technology can help retain and attract practice staff
- ByPolk & Associates
- Feb, 18, 2022
- Health Care
- Comments Off on Confronting the Great Resignation: How technology can help retain and attract practice staff
As businesses continue adapting to the COVID-19 pandemic, many professionals have been questioning their career choices and priorities. This movement, known as the Great Resignation, shows no signs of slowing down. The Bureau of Labor Statistics reported that 4.5 million Americans quit their jobs in November 2021, surpassing the previous record of 4.3 million departures, which […]
Uncovering the secrets to success in physician private practice
- ByPolk & Associates
- Feb, 18, 2022
- Health Care
- Comments Off on Uncovering the secrets to success in physician private practice
Kathleen Blake, MD, MPH, a senior adviser to the AMA on practice sustainability, discussed the results of an AMA-sponsored study that probes the ups and downs among high-performing, physician-owned private practices during an episode of “AMA Moving Medicine.” Although there are fewer physician private practices around now than a decade ago, 49.1% of doctors either own or are […]
3 Ways To Increase Efficiency in Your Practice
- ByPolk & Associates
- Jan, 13, 2022
- Health Care
- Comments Off on 3 Ways To Increase Efficiency in Your Practice
Let’s look now at 3 ways to increase efficiency. Dental practices are businesses and businesses that are more efficient are more successful. As practices move through the natural evolution, they typically end up being less efficient over time. This is often compensated for by the hiring of additional team members, and while it may be […]
How to Ensure You Have a Successful New Year
- ByPolk & Associates
- Jan, 13, 2022
- Health Care
- Comments Off on How to Ensure You Have a Successful New Year
It’s January, the beginning of a year of goals, dreams, changes, updates, and resolutions. There’s actually a designated day in January named National “Ditch New Year’s Resolution Day.” The truth is, that means that less than one in 24 New Year’s resolutions, or rather less than 4% of New Year’s resolutions we make are ever […]
Automating ‘high level’ healthcare tasks can create high value savings
- ByPolk & Associates
- Apr, 10, 2021
- Health Care
- Comments Off on Automating ‘high level’ healthcare tasks can create high value savings
With the recent influx of data across the healthcare industry, the time to fully implement artificial intelligence and machine learning is now, according to Brandon Sim, the chief technology officer and chief operating officer at ApolloMed, a tech-powered healthcare management company. “Especially because recent CMS regulations are going to force electronic health record companies to […]
Why back-office systems are more critical to healthcare providers today than ever before
- ByPolk & Associates
- Feb, 26, 2021
- Health Care
- Comments Off on Why back-office systems are more critical to healthcare providers today than ever before
While healthcare providers have invested heavily in clinical systems over the past decade, they’ve mostly ignored financial and operational systems.
Automating revenue cycle on the back end improves patient engagement on the front
- ByPolk & Associates
- Nov, 24, 2020
- Health Care
- Comments Off on Automating revenue cycle on the back end improves patient engagement on the front
For one health system, robotic process automation equates to about 27,000 hours in a month saved, which correlates to around $500,000. Revenue cycle directors are seeing a clear path for automation to increase revenue, decrease denials, speed up prior authorization and claims, and remove many of the repetitive clicks that hamper daily operations. From an ROI […]
What is funneling, and how can it work for your dental practice?
- ByPolk & Associates
- Feb, 27, 2020
- Health Care
- Comments Off on What is funneling, and how can it work for your dental practice?
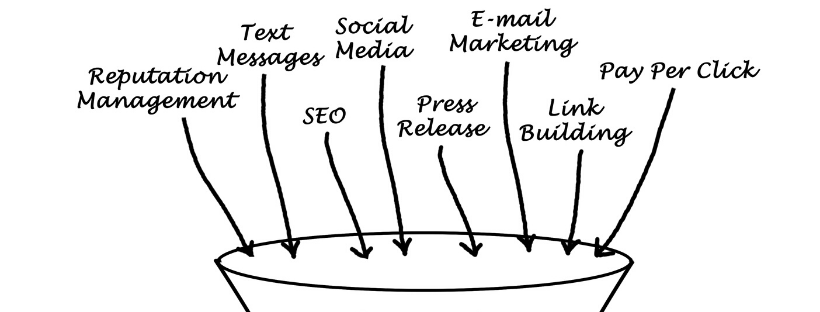
Funneling is a campaign designed to draw in potential patients so they learn about your dental practice and its services. Shay Berman says once patients show interest, you keep funneling so that they want to make that all-important appointment.
How to calculate ROI for dental technology
- ByPolk & Associates
- Feb, 27, 2020
- Health Care
- Comments Off on How to calculate ROI for dental technology
Dr. Chris Salierno reminds dentists they don’t have to rely on their instincts to make big investment and technology decisions. Calculating an ROI formula can work wonders in determining how a practice’s dollars should be spent. Get started now.









You must be logged in to post a comment.